Reflecting on the African Health Strategy
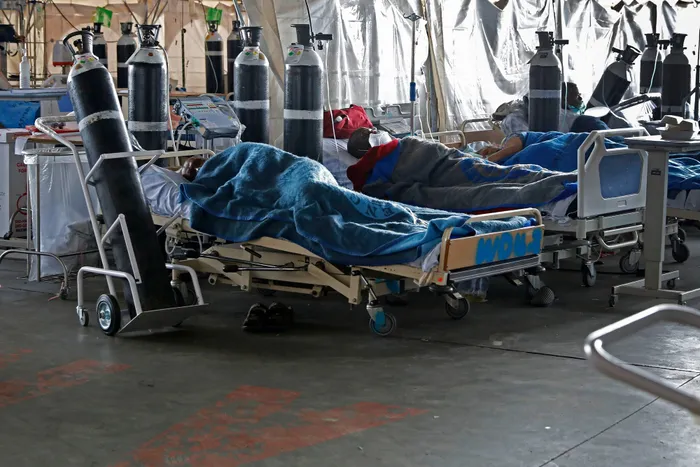
Picture: Phill Magakoe / AFP - Patients are seen lying on hospital beds inside a temporary ward dedicated to the treatment of possible Covid-19 at Steve Biko Academic Hospital. The pandemic complicates issues exposing the fragility of many health systems’ preparedness in responding to epidemic outbreaks, says the writer.
By Njabulo Banda
The United Nations (UN) adopted the Sustainable Development Goals (SDGs) as a call to end poverty and ensure global peace and prosperity by 2030. Indeed, structural violence has manifested in different forms, including a lack of access to health facilities.
SDG 3 stands for health and well-being; however, global averages conceal the uneven progress in the attainment of goals by several countries. The World Bank estimates that almost 90 million people in the globe are disadvantaged by health expenses every year, and there's a high possibility that up to five billion people will still be unable to access health care by 2030.
With the widening social and economic inequalities, the effects of rapid urbanisation and the continuing burden of HIV, and other infectious and non-communicable diseases, the African Union (AU) is committed to steering an integrated, inclusive and prosperous Africa which is free from the heavy burden of disease, disability and premature death.
Through alignment with global and continental health policy commitments such as Agenda 2063: “The Africa We Want” and the 2030 Agenda for Sustainable Development, the current AU Health Strategy (AHS) 2016 -2030’s strategic objectives have been revised with a mission to
foster the strengthening of health systems, scale up effective and efficient health intervention’s, promote intersectoral action and empower communities through African driven responses. The strategy calls for the AU member states to exercise good leadership and effective governance and ensure the enhancement of sufficient financial capacity, human resources and health commodities, all of which are building blocks for health systems strengthening (HSS), as reiterated by the World Health Organization (WHO).
Strengthening of health systems
Despite the guidance from the WHO, the bulk of health initiatives mostly funded by global partners like the US President's Emergency Plan for Aids Relief (PEPFAR) and the Global Fund has maintained a disease-focused approach such as the fight against HIV/Aids, TB and Malaria. Though the life-threatening effects of these pandemics are undeniable, research increasingly shows the decline in incidences and improved clinical health outcomes, especially with regard to HIV. This
translates to countries having the capacity to expand their focus beyond diseases and divert their commitments towards prevention and systems strengthening. Furthermore, the Covid‐19 pandemic complicates issues by further exposing the fragility of many health systems’ preparedness in responding to epidemic outbreaks. Governments were challenged to re-organise facilities and mobilise resources in response to the threats of rising infections.
In South Africa, the already burdened health system resulted in long queues of clients stretching onto the streets outside the health facilities, as clients waited to be screened and triaged accordingly. Despite all these efforts, many essential workers found themselves contracting Covid-19, some even multiple times.
In Nigeria, the health system’s key pains were found around testing capacity, insufficient health workforce, infection prevention and control, health information and insurance, and governance. Closing these gaps to meet the SDG 3 health targets calls for countries to spend a minimum of 1% of their gross domestic product (GDP) on primary health care, according to the World Bank.
A notable scarcity of reliable monitoring tools leads to a limited ability to evaluate countries’ approaches to HSS. Consequently, the African Health Initiative (AHI) partnerships in five sub-Saharan African contexts (Ghana, Tanzania, Rwanda and Mozambique) have opted to utilise an innovative project designed to address key health systems constraints and improve service delivery and health outcomes. The primary aim of this initiative is to stimulate research across the five partners, compile, compare and disseminate findings for programming purposes, as well as policy and HSS strategy formulation.
Effective health interventions: Health Financing Universal health coverage is often confused as a corporate priority and activity. As a result, member states are required to analyse their budgets and determine where to allocate external funding as a means to achieve inclusion for all citizens.
Hence, it is no surprise that the recent incident of one of SA’s health MECs in Limpopo, who ridiculed a Zimbabwean patient in hospitals, telling her to get treatment in her own country, received much criticism from partners, opposition political parties and the Pan-African Parliament.
The SA National Department of Health, though not condoning the behaviour, attributed the MEC’s outburst to an overburdened health system, aggravated by high numbers of undocumented migrants, asylum seekers and refugees from neighbouring countries.
The Pan African Parliament was more explicit in stating their disapproval that such conduct contradicts the spirit of Pan-Africanism and regional leaders’ aim to adopt a regional approach to healthcare and wellbeing.
Intersectoral action and multi-country collaboration
Multi-sectoral partnerships are critical for addressing socio-economic and environmental determinants of health and well-being. One facilitator whose impact is often overlooked, is health information.
Strategic health information and data are of particular importance to investors because these provide the necessary information for planning and decision-making. In this way, healthcare funding initiatives may align with the interests of the funders. African communities need health information that promotes healthy lifestyles, self-care and management.
Researchers, policymakers and programme developers concur that successful health promotion interventions are those which are informed by epidemiological studies and health determinants of the context in which they are implemented, thus, incorporating social, cultural and economic influences.
Empowering communities
Central to the empowering of communities is the need to observe rights-based and gender-sensitive approaches in addressing inequalities that affect beneficiaries, particularly marginalised groups such as women, adolescents and youth.
There is growing attention given to youth health, as performance indicators reveal certain unique risks and vulnerabilities to youth and adolescents. In Africa, these are exacerbated by domestic violence, teenage pregnancy, substance abuse, depression, suicide, and inadequate access to sexual reproductive health.
These social ills threaten the future of young people and, thus, the future African leaders. A major contributor to successful youth health would be the implementation of programmes that are designed with the involvement of young people and informed by their needs.
Ironically, African governments are predominantly still led by older men and fewer women and young people. As will be further deliberated during the Institute for Pan-African Thought and Conversation’s forthcoming AU@20 symposium, scheduled to hold in Pretoria, November 2-4, 2022, progress in the achievement of AU strategic objectives requires deliberate and relentless efforts and a multi-national approach to addressing health not just as the absence of diseases or illness; but rather as the state of complete physical, mental and social well-being.
Dr Njabulo Banda is a Post-Doctoral Research Fellow at the Institute for Pan-African Thought and Conversation (IPATC), University of Johannesburg.