Socialist Movement of Ghana calls for urgent public health response to new malaria threat
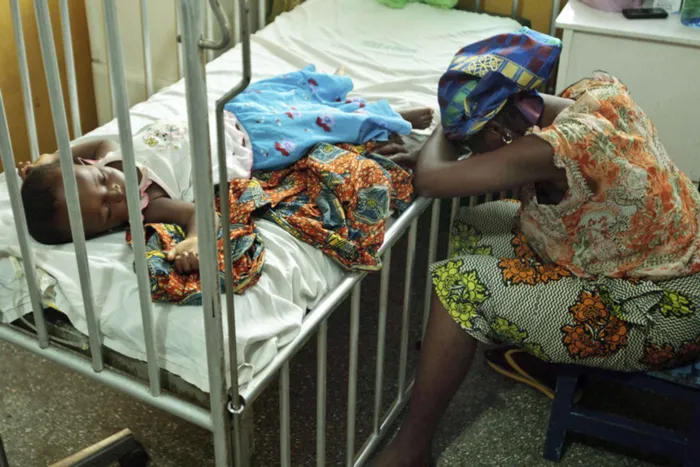
Picture: ANA files – Hassana Ousmane rests her head against the bed where her 21-month-old daughter Zeinab, suffering from malaria and diarrhoea, rests at the Princess Marie Louise Children's Hospital in Accra, April 25, 2012. The invasive, malaria-transmitting Anopheles stephensi mosquito has been detected in Ghana for the first time, the writer says.
By Tanupriya Singh
Health concerns have grown in Ghana in recent weeks following the discovery of a new invasive malaria-transmitting mosquito vector. The Ghana Health Service (GHS) confirmed the presence of the Anopheles stephensi (An. stephensi) mosquito in a statement on April 15, after it had been detected during routine countrywide malaria surveillance in March.
The species was found in samples taken from the Tuba and Dansoman areas of the Greater Accra region. While the mosquito is native to parts of southern Asia and the Arabian Peninsula, it was first detected in Africa in Djibouti in the Horn of Africa in 2012. It has since been identified in Ethiopia, Somalia, Sudan, Nigeria, Kenya, and now Ghana.
The Accra Collective of the Socialist Movement of Ghana (SMG) has called for “proactive measures to implement effective environmental management practices”, warning that a “robust mosquito species poses a significant concern” as it could potentially lead to an increase in the mosquito population in the country and result in a greater threat of malaria transmission.
“Because malaria causes so much illness and death, the disease is a great drain on many national economies,” the collective said in a statement. “Since many countries with malaria are already among the poorer nations, the disease maintains a vicious cycle of disease and poverty.”
Malaria continues to pose a serious, and often fatal, health risk to people across the African continent. According to the World Health Organisation’s (WHO) 2022 World malaria report, there were 247 million cases of malaria globally in 2021, with an estimated 619,000 deaths.
The WHO African Region accounted for 95 percent of all cases and 96 percent of all deaths, with about 80 percent of fatalities recorded among children under the age of five. Nigeria, the Democratic Republic of Congo, Tanzania, and Niger have been the worst affected.
According to Ghana’s National Malaria Elimination Programme (NMEP), the country recorded over 3.7 million confirmed cases of malaria infections and 120 deaths between January and September, 2022.
While malaria is endemic in the country (and the Continent), An. stephensi might pose new challenges for disease surveillance and control. Research indicates that while malaria has traditionally been prevalent in rural areas in Africa, the new species’ population establishes itself in urban areas. Though the species has been found to have a low propensity to bite humans, it could play a key role in local settings and periodic outbreaks, according to research conducted in Djibouti.
The species’ spread to other cities on the African continent could possibly put at least 126 million people at risk.
An. Stephensi was a “unique” vector, the GHS stated, capable of breeding in a wide range of sources, ranging from ponds and swamps to artificial human-made water storage containers including tanks and sewers, which are prevalent in urban areas.
This also raises questions of the links between the spread of malaria-transmitting mosquitoes and urban planning, including water and sewage infrastructure especially for urban poor communities, who, additionally, may not also have proper access to health care. These linkages between class and health, or what is more broadly understood as the social determinants of health, were also highlighted during a discussion hosted by Pan African Television on April 19.
Moreover, while dry seasons offered a brief respite in the form of a decline in malaria cases, this may change with this new species, given that it can survive in very high temperatures, adapt to different climates, and spread fast, the GHS has said.
The species has also been found to be resistant to “multiple insecticide classes in many locations, including Africa, posing challenges to its control”. The GHS has announced the establishment of a task force to implement measures to contain the spread of the species, including the removal of water collection points in the vicinity of homes and communities.
Just days before the GHS statement, Ghana also became the first African country to approve an experimental malaria vaccine for public use. Called the R21/Matrix-M vaccine, it has been developed by the University of Oxford and manufactured by the Serum Institute of India.
Meanwhile, the SMG has urged the Ghanaian government to take adequate steps to address the risks associated with the new species.
Speaking on behalf of the Accra Collective during the Pan African Television discussion, Bernard Senyo Nyendu called on the government to send out information to the public and for political leaders to release necessary resources, emphasising the need for a multisectoral approach involving various stakeholders.
The need for stronger alert systems and information dissemination was also highlighted by Dr Nii Lante Blankson, a physician specialist.
The Accra Collective has also called for the strengthening of disease surveillance systems and greater investment in health care, and for the GHS task force to be a task force “for the people”.
Importantly, it has pushed for a revival of consultations between Ghana and Cuba for a malaria eradication project that “was abandoned”. In 2014, Ghana had signed a letter of intention with Cuba’s biological laboratories enterprise, Labiofam. A joint malaria programme had been implemented in Accra, and the accord signed also included technical advice and the provision of biological products.
Strengthening disease response mechanisms inevitably raises questions of funding. “This is about more than malaria. This discussion is also about the state of our economy,” SMG general secretary Kwesi Pratt Junior said.
“When we are told that we are spending about 70 percent of total national revenue on paying debts or paying the interest on debts, and that we need about 128 percent [of revenue] to pay for the debts and to pay for the public sector, it simply means that there is no money [left] to fight disease.”
Tanupriya Singh is a writer at Peoples Dispatch and is based in Delhi.
This article was first published on Peoples Dispatch