One call away from a stronger health system: learnings from Malawi’s ‘health centre by phone’
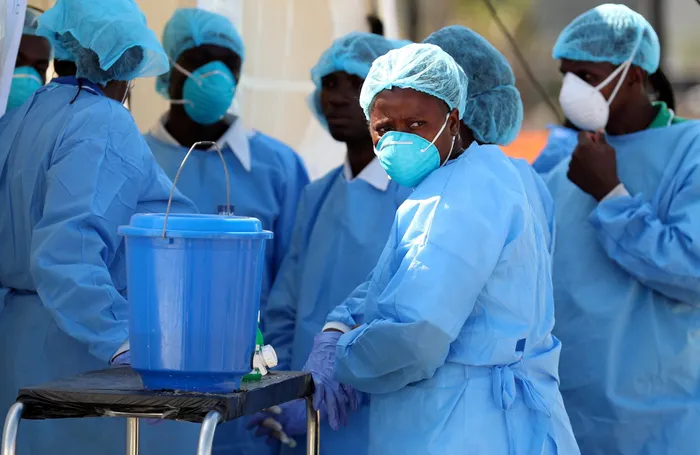
Picture: Malawi faces its deadliest outbreak of cholera to date. Since it began in March 2022, the country has reported more than 40,000 cases and 1,400 deaths.
By Hope Ngwira, Claudia Shilumani, and Adrian Chikumbe
Imagine your young child is not feeling well. With recent news reports about an outbreak of cholera spreading throughout your community, you’re nervous about their potential of being infected. But the nearest health centre is hours away, and you need a referral from a certified health provider to see an infectious disease or paediatric specialist.
This is a reality for many Malawian parents right now, as the country faces its deadliest outbreak of cholera to date. Since it began in March 2022, Malawi has reported more than 40,000 cases and 1,400 deaths.
In a health system that’s been weakened and overburdened by the pandemic, responders had to find new ways to quickly deliver accurate, individualized health information to people in need.
Malawi is taking an innovative approach to this challenge – and other countries have much to learn from their experience.
To get connected to health professionals fast, Malawians can call the “health centre by phone,” Chipatala cha pa Foni (CCPF). It’s a free 24/7 national health hotline that anyone can use to receive information, counsel, and referrals from a certified nurse, no matter where they live in the country. Data from the calls also keeps the Ministry of Health up to date on the latest health trends circulating at the local level, helping them monitor and respond to any misinformation or surges of cholera.
Malawi is not the only country that has a free health hotline, but CCPF is one of the first in Africa to be government-run at the national level. Since the Ministry of Health took over full ownership of the hotline from the non-profit VillageReach in 2020, the platform has grown even more, with calls increasing five-fold over the past two years to nearly 110,000 interactions each month.
Recently, a high-level group of government, NGO and donor partners from South Africa visited Malawi to learn from the CCPF initiative and to share lessons from their own experience with a countrywide Covid-19 hotline. Hosted by Malawi’s minister of Health, the trip was an opportunity for both countries to exchange learnings about building a sustainable, fit-for-purpose health hotline that can expand to issues beyond outbreak response.
What emerged from this dynamic process were three key learnings that can be applied to expand telehealth and contribute to health systems strengthening more broadly across the continent.
First, strong government stewardship is critical to scale. Once the Ministry of Health took over full operations of the hotline, CCPF was integrated into the national health system and has helped advance Universal Health Coverage across Malawi.
The government’s strong endorsement of the initiative also strengthened the perception of CCPF as a reliable source of health information. For new health programmes to succeed and grow, it is essential they be led by or have strong support from the national government.
Second, it takes a village, including private sector partners, to ensure sustainability. CCPF has only been made possible through a strong partnership between the Malawi Ministry of Health, VillageReach, GIZ, USAID, Viamo, and the private phone network Airtel.
Using innovative financing mechanisms to bring on private partners was key to CCPF’s longevity. To transition from reliance on donor funding, organisations and governments looking to scale should develop investment cases for health programmes that give private sector partners incentive to engage.
Lastly, health equity must be considered both from the provider and patient perspectives. While health hotlines are open to anyone who wants to call in for health advice, not everyone uses the service equally.
In Malawi, more men have cellphones, and can access CCPF more easily. Meanwhile in South Africa, more women call the Covid-19 hotline than men. These insights remind us that all health programmes must consider how to better reach all people, regardless of gender, age, or ethnicity.
Mozambique, the Democratic Republic of Congo, and Libya are implementing their own national health hotlines, with VillageReach’s support. The organisation is also linking partners to each other to establish a community of practice, so countries like Nigeria, Kenya, and Côte d'Ivoire can take inspiration from Malawi’s Chipatala Cha Pa Foni to inform their own telehealth strategies.
With the cholera outbreak spreading in Mozambique, South Africa, the Democratic Republic of Congo, Kenya, and Nigeria, this kind of cross-country learning and partnership is more important now than ever.
We must continue to invest in expanding innovative solutions, like health hotlines, to extend our reach to the farthest communities.
We must accelerate efforts to strengthen our health systems so that we can better respond to ongoing emergencies and stand resilient in the face of the next crisis.
And we must leverage our collective experience and look to each other to share and implement learnings that will strengthen all health systems and secure healthier futures for all people.
Hope Ngwira is Senior Manager for Advocacy and Communications in the Malawi office of VillageReach. Claudia Shilumani is Vice President of Partnerships & Impact at VillageReach, with offices in Malawi, Mozambique, the Democratic Republic of Congo, and the United States. Adrian Chikumbe is a Spokesperson for the Malawi Ministry of Health of Malawi.